I am an IBCLC (International Board Certified Lactation Consultant) in private practice in Northern Ireland and a La Leche League Leader with La Leche League of Ireland
How does an IBCLC consultation differ from support at a breastfeeding group? Why would I book one?

When we have our first baby it often seems like we’ve suddenly dropped into a world that we never knew existed before. A world of baby classes, and books and online support and baby experts. The same is true for breastfeeding. So many mums tell me that they assumed that when their baby was born they would just go to the breast and everything would click into place and that they didn’t realise there was so much to know about breastfeeding. Many of us find this. Suddenly a whole world of baby feeding emerges before us. Our families give us information. Our HCPs give us information. We discover breastfeeding support groups, and online support groups and through these we find layers of knowledge and support - Peer Supporters, Breastfeeding Counsellors, midwives, Drs, IBCLCs - each providing slightly different roles. For some of us breastfeeding does click into place, but the vast majority of us do hit some obstacles in the early weeks and need some extra support. When this happens you may hear the term IBCLC for the first time, and someone may suggest that you see one, or tell you their experience of seeing one, and you may be curious about what an IBCLC is and what happens at a consult. What is different from getting support at a group?
What is an IBCLC
An IBCLC is an International Board Certified Lactation Consultant. It is the gold standard of breastfeeding support throughout the world. An IBCLC has either come from a health professional background or has received university level education in 16 specific health subjects (e.g. anatomy,physiology, infant development, nutrition, psychology or counselling, sociology or social anthropology amongst others ). After this they have received at least 90 hours of specific breastfeeding training, and have completed many hours of clinical experience. The routes available in the UK and Ireland to quality will usually mean there are at least 1000 hours of clinical experience (providing breastfeeding support). Then they have passed a 4hr exam to gain the IBCLC accreditation, which is given by the IBLCE exam board. In order to maintain certification they need to continue to have at least 75 hours of training every 5 years.
An IBCLC is the expert on breastfeeding, and can help with all aspects of feeding, from managing slight tweaks to feeding in a healthy full term baby, to helping babies with complex health conditions, and everything in between. IBCLCs may work in hospitals (many of our hospital infant feeding coordinators in NI are IBCLCs), some may work in the community within the NHS (HVs and midwives may refer issues to them), and others work in private practice. I am an IBCLC who works in private practice. This means I work outside of the NHS, seeing families in their homes at a time that works for them and I am able to spend up to 2 hours with a family in a breastfeeding consultation.
Why would I want an IBCLC consultation? Can’t I get all the support I need for free from the NHS and voluntary support groups?
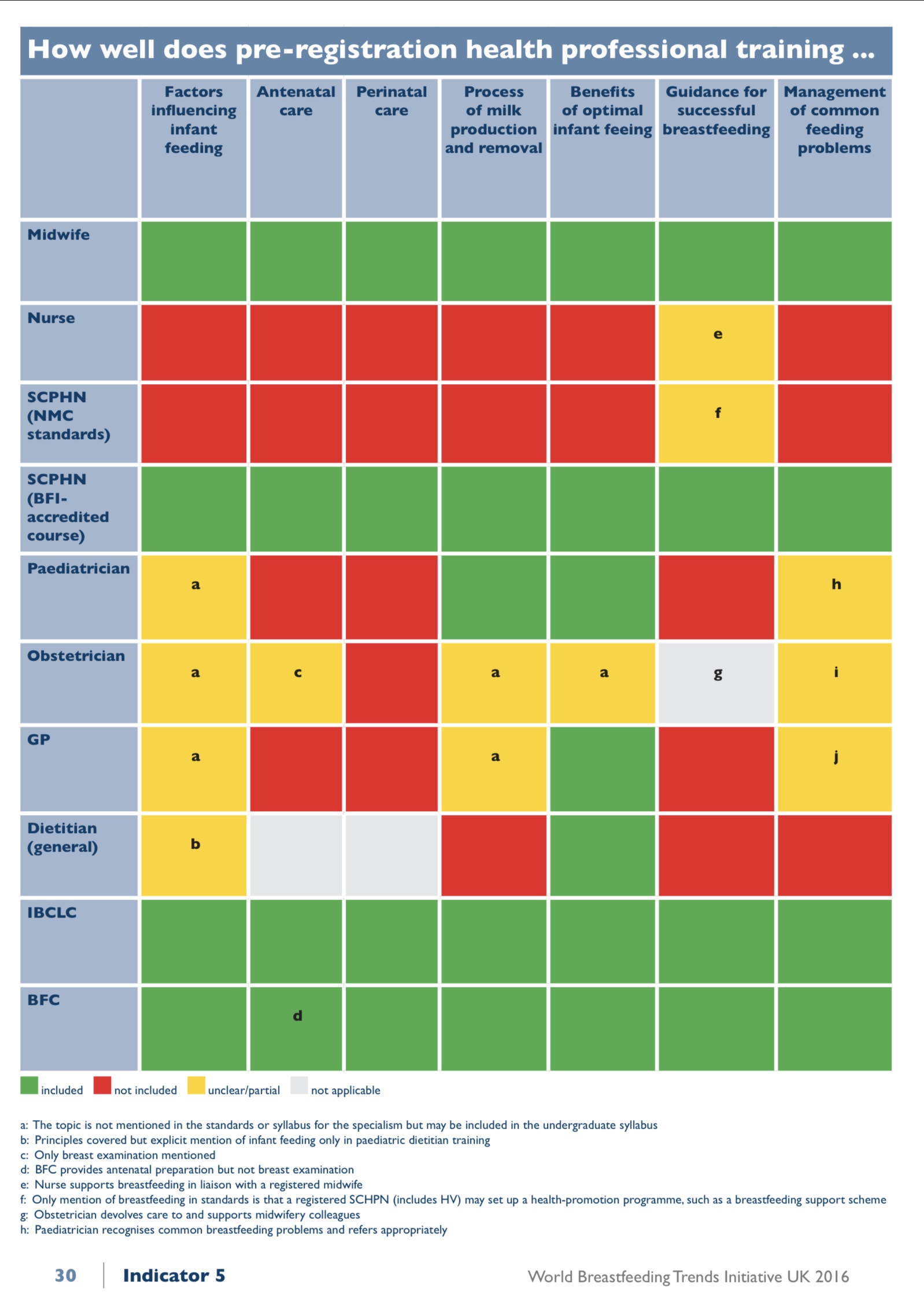
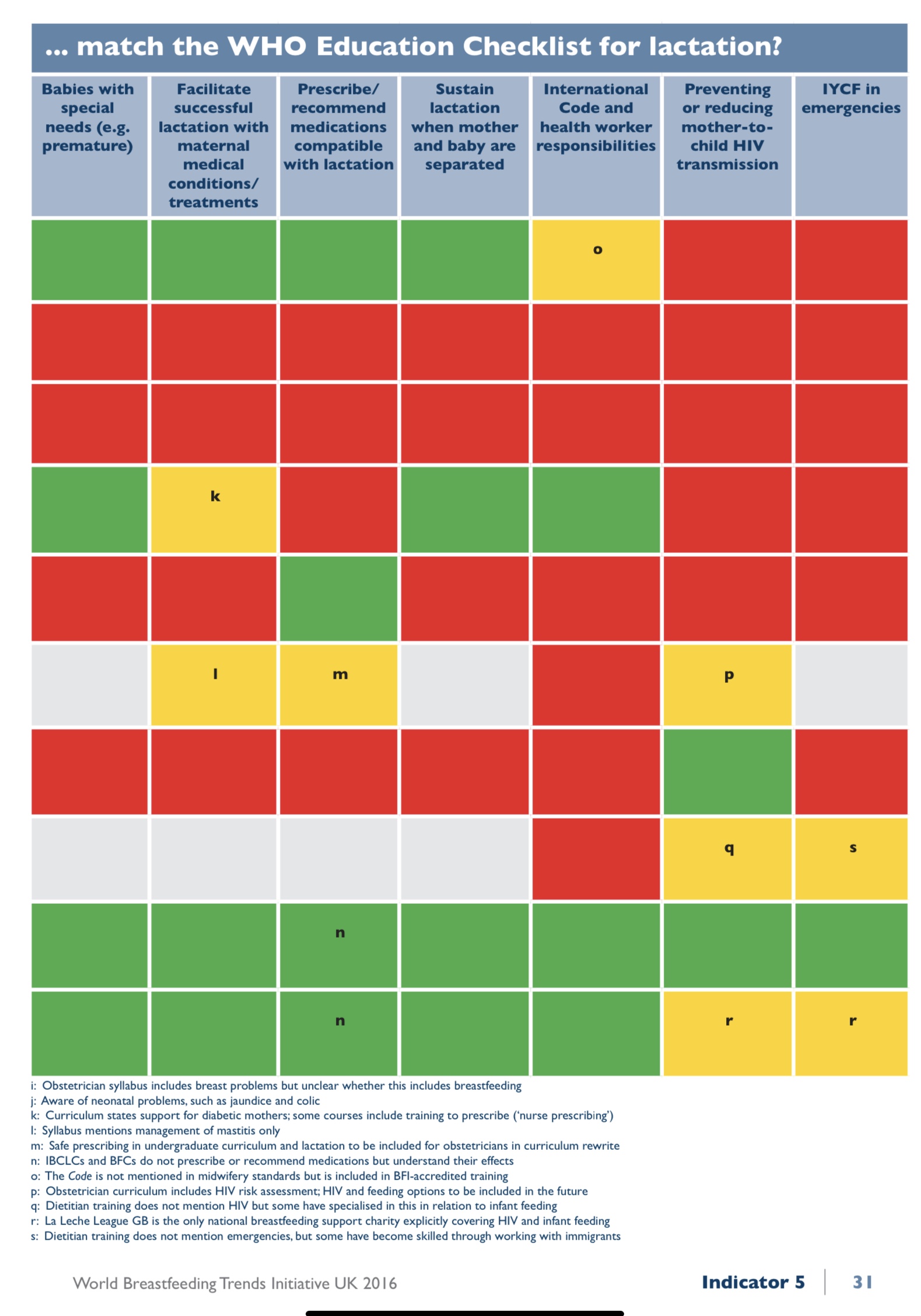
The answer to this is very individual, and will depend on what you want from breastfeeding support and what issues you are having with feeding, and perhaps the kind of support you have had in the past. Ideally families don’t need an IBCLC. Ideally they will have had good breastfeeding information before giving birth, and are well prepared. Ideally their birth goes well, and they just need a few tips and hints from their midwives and friends and family to get them on their way, but we don’t live in an ideal world. In reality, most of us hit problems. The support we get from the NHS and from voluntary support is often fabulous, but not always. It very much depends on circumstances. It may depend on where you live, what groups are available, who runs them, and what caseload your midwives or HV have. It may depend on how common breastfeeding is where they work, and how this affects their ongoing skills. Sadly, it may also depend on their own attitudes and experience with breastfeeding and if they value it. It may depend on what kind of problem you are facing. Someone with simple positioning issues may get great support. Someone else may have problems which don’t resolve with this support and they need someone with more knowledge. In 2016 the WBTi UK (World Breastfeeding Trends Initiative) published a report looking at breastfeeding support in the UK and found significant gaps in training. Below is an image of the training gaps they found. The row referring to SCPHN would be a Health Visitor. You will see there are 2 rows for SCPHN - for BFI accredited and non BFI accredited courses. As yet we do not have any BFI accredited training courses for SCPHNs in Northern Ireland.
The bottom row (BFC) refers to breastfeeding counsellors. This would be voluntary counsellors such as those in La Leche League or NCT for example, or Cuidiu in ROI.
What’s the difference between the support at an IBCLC consultation and a breastfeeding support group?
Not all support groups are equal. Some support groups will be led by a peer supporter (someone who has fed their own baby for 4 months and had some training in supporting others with common issues). Some will be led by Health Visitors (training shown above). Then there are voluntary support organisations like La Leche League with extremely skilled counsellors (see training above). I can’t recommend organisations like this highly enough. I trained with LLL before becoming an IBCLC and I still volunteer as a BFC with them. I gained so much as a new mum, and I love giving back and seeing other mums gain from the group too. Support groups are a fantastic way to get support, to get information about breastfeeding, to get some specific help if you need it, to hear the issues the others are having and how they might approach them, to meet new mums and to get parenting worries off your chest. They are wonderful, but they are not the same as an IBCLC consult. Think of the support you get at a meeting as ‘broad’ and the support you get at an IBCLC consult as ‘deep’.
At a support meeting there will be multiple mums there, probably many of them needing help and there may only be 1 BFC there to help. Large groups may have more than 1. The BFC will likely be limited in time with each mum, and needs to also attend to the general facilitation and running of the group. This means there is usually not time to work on complex issues. The support is broad and wide, dealing with lots of issues across many mums but not able to deal with an individual mum for an extended period. In addition there are things that a BFC is simply not trained or insured to do, like assessing tongue movement.
The support at an IBCLC consult is deep and specific and individualised. An IBCLC will usually spend up to 2 hours with a family, in their own home. This allows you to spend time looking in depth at whatever is concerning the family, or whatever is causing distress. It allows you to look at feeding in your own environment, why specific pillows or chairs may not be working particularly well and what might work better. It allows mums who can’t drive after a C-section to get support in their own home. The time allows you to look at an entire feed, and often to look at more than one feed in a young baby. It allows time to look at expressing, and to check the fit of flanges or nipple shields - something much more difficult in a public setting like a cafe where many support groups are held.
An IBCLC consult can look at much more in-depth issues and provide extremely tailored and specific care to you. A BFC is trained to provide support for things that happen in the normal course of breastfeeding, whereas an IBCLC can provide support when issues drift outside of that. Take low weight gain for example. A BFC can give support for a low gaining baby who is a little below average and needs a few tweaks to feeding. A baby who is dropping through centiles however needs targeted support and a care plan around extra volumes of milk that may be needed, how this might be given and how to wean it out again if possible. An IBCLC will provide an individualised care plan for you, and will provide follow up for that plan after the consult.
Crucially though the difference is individual focus on you and you alone. An IBCLC consult is entirely focused around what you want for that 2 hours... the questions you have, the issues you have, and how you want breastfeeding to look for you.
What happens at an IBCLC Consultation?
I can describe what happens at one of my consultations - I think others will be pretty similar. When you book a consultation, I will probably ask for some general information so that I can prepare. If you book online I will usually contact you by email shortly after booking. It might be information about your baby’s age or weight, or some specific questions about any problems you have listed when you booked. I might suggest that you think of all the questions/worries that you have so that you can make a list of them for our meeting. I want you to get the most out of that meeting. I want you to make use of me in the way that is best for you when I’m with you. So if you have a dozen random queries about feeding or baby behaviour (sleep, baby noises, baby movements etc etc), or have been told several conflicting things from people, then it’s a chance to discuss all of them and having a list means you don’t forget them.
We can look at anything regarding your baby and feeding. My consults in just the last couple of months have been booked to look at:
Painful feeding /latch issues / Clicky feeding
Recurrent mastitis / blebs
Relactation
Low weight gain / Concerns about low milk supply
Oversupply/excessively high weight gain / Concerns about fast letdown
Unsettled /colicky behaviour
Reflux
Managing breastfeeding with allergies
Constipation /Green Poo / other concerns about nappies
Transitioning from nipple shields
Tongue tie
Breastfeeding preparation antenatally
Managing tandem feeding
Reducing formula and working towards exclusive breastfeeding
Managing breastfeeding multiples
General breastfeeding check for newborn
Vasospasm
Pain on one side only
Fussy at breast
Starting expressing and offering bottles
Sleepy baby at breast
Exclusive expressing
Transitioning baby from bottles to breast and vice versa
Returning to work
Starting solids
Sleep Patterns
Non latching baby
Bottle refusal
Fertility
Most consults also touch on what’s expected baby behaviour developmentally, routines and differing advice you may have heard, so it’s a chance to talk about anything you need.
When I arrive I usually start by reviewing everything that has happened so far, what you want to get out of the consult, how you would like things to look for you, what concerns you have about your baby etc. When your baby is ready we will offer a feed so that I can observe. If your baby is hungry when I arrive then those might get swapped around. We might feed straight away and then chat while your baby is feeding. I often suggest not feeding your baby for an hour before I arrive so that we can be pretty sure that they will feed when I’m there, but I’m well aware that babies are hungry when they’re hungry - not when the clock says so, so we work around whatever your baby needs to do. There’s no point in your baby being so hungry that they are upset!
If you are wanting to try different positions and different rooms then we can do that. We can look at positioning on your chair, your sofa, on your bed. We can look at night time positions like feeding when side lying.
It’s ok for others to be there. Often in consults there are siblings, or both parents, or sometimes grandparents. Anyone you want to be there is ok with me. Sometimes they will have different questions to you, and that’s ok too.
Sometimes I might want to touch you or your baby to watch what is happening or to suggest a little change to positioning. I might want to check your baby’s mouth and see how they are sucking. I might want to lay them down and observe how they move. I will ask your permission before touching you or your baby. I will wear a non latex glove before checking your baby’s mouth. We may weigh the baby to check how weight gain is progressing.
I will take a few notes when I am with you, just to summarise what we are talking about. After the consult I will write up any feeding plan/actions that we have discussed and will send it to you. I will follow up with you a few days later to see how the plan is going. If you have any questions that come up before I get back to you, you can contact me at any time. Part of your consult fee includes this follow up.
There is never any need to apologise to me for the tidiness or otherwise of your house! I have children! I am well aware that after children arrive in your family, the way you had your house beforehand may never be the same. I’m also well aware that you may have just given birth days or weeks previously and that new babies are all consuming. The only thing I am focused on is you and your baby, and whatever is causing you worry or distress. That’s my only concern.
Is an IBCLC consultation expensive?
This probably depends on the value that you place upon it. Yes you get free support through the NHS, and through voluntary groups. What you are paying for in a private consultation is time, expert knowledge, experience, and an individualised service. In fact the cost is probably not that different from what the NHS would cost for a similar service. As far as I understand a Health Visitor in the NHS starts on the Band 6 pay scale. The hourly rate is £15.55-19.06 for a Band 6 according to the NHS employers website (at time of writing). The infant feeding coordinator in a hospital (who may be an IBCLC) is likely a band 7, earning £19.22-22.39 an hour. When you get time with your HV or NHS community based IBCLC you are very unlikely to get 2 hours with them in your home, but if you did what would the cost be to the NHS?
When I see families I usually spend 1-2 hours travelling on the round trip. Even just going a small way across a city can take 30 mins, and then there is the return journey. My free travel area is 20 miles, and that will normally take around 30 mins. So let’s assume a 30 min journey each way and look at costs, and assume that we’re paying for someone with at least the pay grade of a band 6-7. We’ll assume £20 an hour.
Return Journey Travel - £20
2 Hour Consult - £40
So the HCP will be paid £60 for the 3 hours it took them, but that’s not the cost of the consult. It will cost more than that to the NHS who is paying for the full consult. In addition to the £60...
That HCP will have a set of scales which were bought and need regularly calibrated - at a cost.
They may have an iPad or other tablet for electronic records - at a cost.
The NHS will be paying for the ongoing training of that HCP.
They will pay for the computers and software that store those patient records.
They will pay for the HCP insurance
They will pay for the cost of fuel mileage of the trip and possibly wear and tear to the car, or may provide a car lease scheme.
They are paying office costs for the time writing up the visit.
There will be more costs, but these are the most obvious basics. This will come to substantially more than £60
A private IBCLC has to pay for all of this personally, plus admin costs for running a business, all without the savings of the economy of scale.
Now let’s factor in follow up support. In a private consult you get included follow up. This is usually by phone/email for 2 weeks after the consult. If the original problem is not yet involved and we are still tweaking things it might last a little longer. I usually count in an hour for the follow up over those times. So that’s another £20.
On average I spend around 4-5 hours on each consult, plus the additional admin costs. When you count this up, a private IBCLC is no more expensive, and possibly less expensive, than an NHS breastfeeding support professional. The NHS cost is simply hidden in our taxes and the system is so overstretched that you usually do not get the same time and focus that you get with someone in private practice. The fees for my consults are here.
It still might seem like a lot of money, but factor in costs if you stop breastfeeding. You will need to buy formula at a cost of around £400-700 for the first 6 months, plus bottles, steriliser etc, and the time involved in making, washing and sterilising bottles. Alternatively if you count up how much many of us spend on other gadgets and remedies to help our babies (from gripe water and colic remedies to white noise machines and sleep aids) you can easily surpass the cost of a consultation. A consultation is an investment in your breastfeeding relationship when you hit problems.
I’m a strong believer in free breastfeeding support. It’s why I am still involved in voluntary work, but the type of support you get in support groups is simply different than what you get in a private IBCLC consult and there is a place for both. So yes, I believe it is worth it, that it is actually not expensive for the kind of support you get - and I do my very best to provide you with the best possible service that I can. If you need this support and can’t afford my fees, please still contact me as I will try to help and if you need a consult we can come to an arrangement that works for you. I am passionate about helping you breastfeed and that’s my bottom line.
If you think a consult might be for you, please get in touch, or Book A Consult online.
Further Reading
1. Steps for IBCLC Certification - https://iblce.org/step-1-prepare-for-ibclc-certification/
2. WBTi UK Report 2016 - https://iblce.org/step-1-prepare-for-ibclc-certification/
3. Local LLL Groups - https://www.lalecheleagueireland.com/groups/
4. NHS Pay Scales - https://www.nhsemployers.org/pay-pensions-and-reward/agenda-for-change/pay-scales/hourly
Important Information
All material on this website is provided for educational purposes only. Online information cannot replace an in-person consultation with a qualified, independent International Board Certified Lactation Consultant (IBCLC) or your health care provider. If you are concerned about your health, or that of your child, consult with your health care provider regarding the advisability of any opinions or recommendations with respect to your individual situation.
